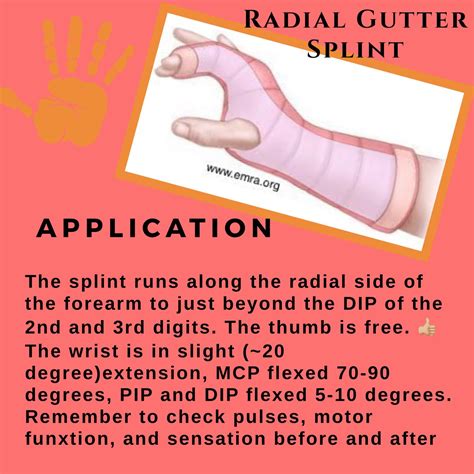
Radial gutter splints, often employed in pediatric orthopedic care, are a critical tool for managing conditions such as distal radial fractures. These splints are essential for immobilizing the wrist and distal forearm while allowing freedom of movement to the hand, thus promoting both healing and maintaining hand function. This article explores the practical application and underlying principles of radial gutter splints, offering a focused guide for medical professionals.
The primary application of radial gutter splints lies in their ability to immobilize two areas simultaneously—the wrist and the distal forearm—without restricting hand mobility. This dual immobilization is particularly useful in treating fractures that occur in both areas but do not involve the hand. Understanding the intricate design and application of these splints is crucial for ensuring both patient comfort and effective healing outcomes.
Key Insights
- Primary insight with practical relevance: Radial gutter splints provide dual immobilization for both the wrist and distal forearm, which enhances healing and maintains hand functionality.
- Technical consideration with clear application: Precision in splint application is essential to avoid undue pressure on certain areas, which could impede blood flow and healing.
- Actionable recommendation: Always perform a thorough assessment of the patient’s anatomical and fracture specifics before applying the splint to tailor it to individual needs.
Understanding the Anatomy and Mechanics of Radial Gutter Splints
Radial gutter splints are meticulously designed to accommodate the specific anatomy of the distal radius, ulna, and the hand. These splints typically consist of two primary sections: one that wraps around the wrist and distal forearm, and another that is shaped to fit the hand. The precise fit is crucial to avoid compromising blood circulation or nerve function. During application, the splint must be molded to the contours of the limb, ensuring that it provides adequate support without being overly restrictive. For instance, in cases where a fracture is present in the distal radius and ulna, but not the hand, a radial gutter splint offers a precise solution that aligns with the bone structure while allowing the hand to remain functional.
Clinical Applications and Best Practices
In clinical settings, the application of radial gutter splints follows a series of structured steps to ensure patient comfort and optimal healing. First, it is imperative to assess the patient’s fracture and overall condition, determining the correct splint size and design. Following this, the splint is wrapped around the limb, ensuring that the wrist is fully immobilized while the hand remains free. It is essential to avoid excessive tightness that could lead to complications such as compartment syndrome. After fitting the splint, a comprehensive review is conducted to check the splint’s fit and the patient’s comfort level. Real-life examples include treating a pediatric patient with a distal radial fracture where a radial gutter splint allowed the child to maintain hand function and engage in necessary daily activities, thereby accelerating recovery and compliance with the treatment plan.
What are the signs that a radial gutter splint may need adjustment?
Signs include increased pain, swelling, or numbness in the limb. If the splint feels too tight or too loose, it should be adjusted to prevent complications and ensure proper immobilization.
How long should a radial gutter splint be worn?
The duration for which a radial gutter splint should be worn varies based on the severity of the injury. Typically, it ranges from a few weeks to several months, depending on the healing progress monitored by an orthopedic specialist.
In summary, radial gutter splints play an invaluable role in the orthopedic management of distal radial and ulnar fractures, particularly in pediatric patients. By understanding their anatomical fit, clinical applications, and adherence to best practices, medical professionals can ensure effective treatment outcomes and promote patient comfort and compliance.